Hair loss is one of the most common concerns in aesthetic medicine, and one of the most misunderstood. While dihydrotestosterone (DHT) is the most well-known driver of androgenetic alopecia, it is far from the only one. Alopecia is a multifactorial condition — meaning multiple biological processes contribute simultaneously to follicle miniaturisation and loss. A treatment strategy that addresses only one of these pathways will always be leaving results on the table.
The earlier treatment begins, the more there is to preserve. Hair loss is far easier to slow than it is to reverse.
The three key drivers of hair loss
1. DHT and follicle miniaturisation
In genetically predisposed individuals, DHT binds to androgen receptors in hair follicles, progressively
miniaturising them over successive growth cycles. The result is a gradual reduction in hair shaft diameter
and length, and eventually follicle dormancy. This process occurs in predictable patterns — receding
hairline and crown thinning in men; diffuse thinning at the crown and widening part in women.
A second inflammatory pathway — mediated by prostaglandin D2 (PGD2) acting on DP2 receptors — compounds
this miniaturisation independently of DHT.
Treatments targeting this pathway: Dutasteride · Topical Cetirizine
2. Reduced scalp blood flow
Hair follicles are metabolically active structures with a high demand for oxygen and nutrients. As we age,
scalp microcirculation declines — reducing the vascular supply that follicles depend on to sustain the
anagen (growth) phase. Poor follicle perfusion accelerates the transition from active growth to dormancy,
and is a significant but often overlooked contributor to hair thinning, independent of hormonal factors.
Treatment targeting this pathway: Minoxidil
3. Mitochondrial decline and cellular ageing
Mitochondria are the energy-producing units of every cell — and hair follicle cells are no exception.
With age, mitochondrial density and function decline, reducing the cellular energy available to sustain
follicle cycling. This manifests as shorter anagen phases, reduced hair shaft calibre, and impaired
follicle repair. Alongside this, chronic low-grade scalp inflammation further suppresses follicle
activity over time. Regenerative therapies that deliver concentrated growth factors and signalling
proteins directly to the scalp can help reverse this decline by stimulating follicle stem cells,
improving the local cellular environment, and promoting anagen re-entry.
Treatment targeting this pathway: LP-PRP
Science
What are the phases of the hair life cycle?
The hair cycle is a recurring process of growth, regression, rest, and shedding — essential for hair to continually renew itself throughout a person's life. Understanding these phases explains why hair loss treatments take months to show results, and why disruption at any stage leads to visible thinning.
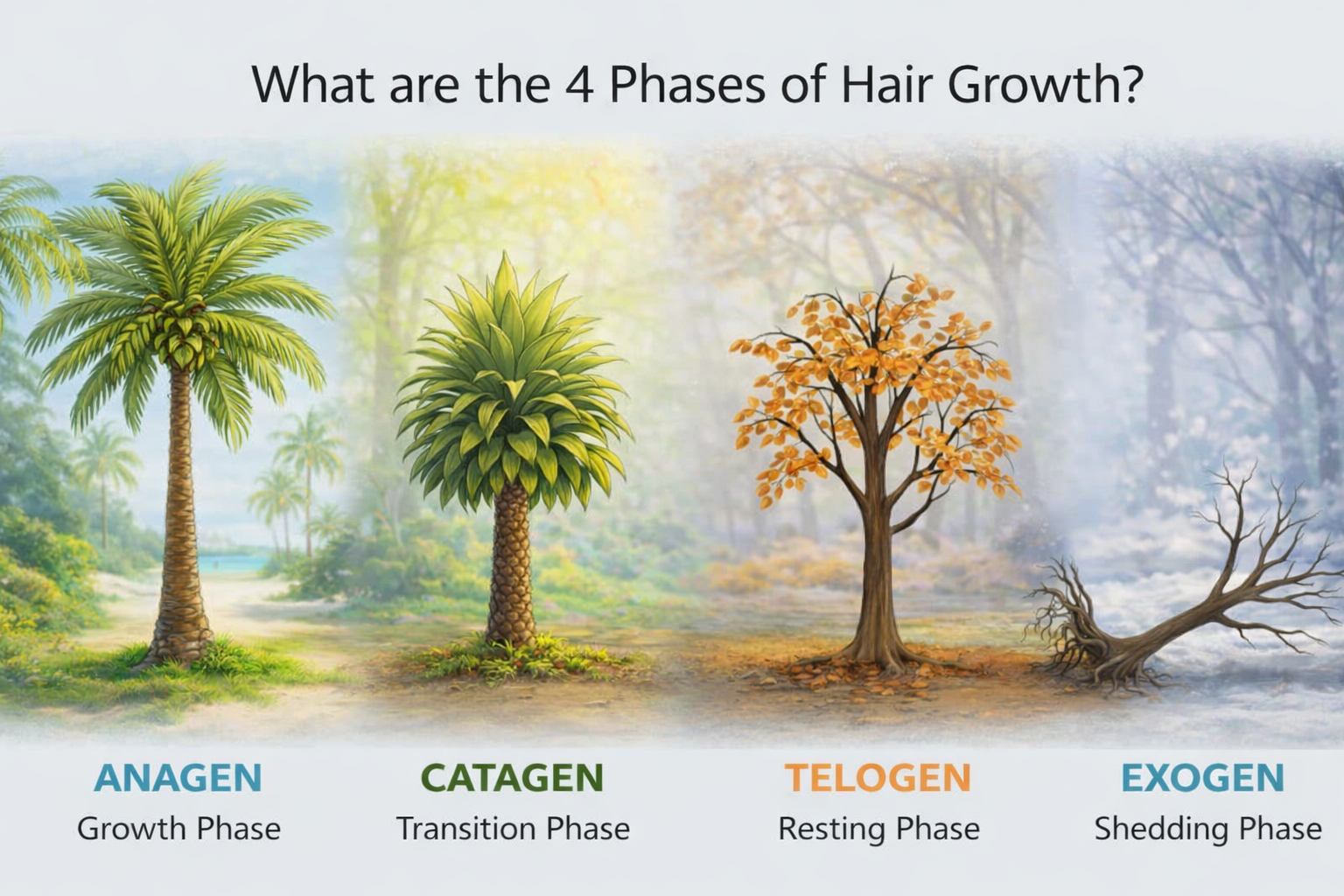
The active growth phase, producing a new hair shaft. Lasts 2–6 years for scalp hair. Around 80–90% of scalp hairs are in this phase at any given time.
A short 2-week transitional phase where the follicle regresses and the hair separates slightly from its base. Only 1–2% of scalp hair is in catagen at once.
The hair rests in the follicle for 2–3 months (~10% of scalp hair). Meanwhile, a new hair begins growing beneath, ready to replace it.
The old hair sheds — typically 50–100 hairs per day. Brushing and washing assist this natural process, which can span several months.